Who Is Not Eligible For Covered California
Immigrants who are not lawfully present do not qualify for a health plan through Covered California however, they may qualify for coverage through Medi-Cal up to age 19 or for pregnancy coverage. Immigrants who are not lawfully present can also buy private health insurance on their own outside of Covered California.
Q Can I Have Both Medicaid And Medicare At The Same Time
A. It depends. If you receive Supplemental Security Income from the Social Security Administration, you are automatically eligible for Medicaid and often receive Medicare as well. If you receive both Medicaid and Medicare, Medicaid will pay your Medicare premium, co-payments and deductibles. If you have both Medicare and Medicaid, you should show both cards to your medical care provider each time you receive services. Resources for Those Who Have Medicare and Full-Benefit Medicaid
Do We Qualify For Medicaid Or Chip
The Medicaid income guidelines vary by state so look up your state on our Kids Health Report and scroll to the Who Qualifies section to see specific income guidelines for children, pregnant women and parents. We are in the process of adding state income guidelines for adults without dependent children but, in the meantime, you can check this spreadsheet for that information.
Don’t Miss: What Day Does Unemployment Get Deposited In Nc
Department Of Financial Services
Health insurance is a very important protection for you and your family. Aside from providing coverage for services related to an existing illness or a sudden, unexpected illness, it may also provide coverage for important preventative care to detect illnesses before they become serious. Since many families obtain their insurance coverage through an employer, it is important to know your insurance options should you become unfortunate enough to lose your job.
What Is The Minimum Income To Qualify For Covered California
The federal threshold is 400 percent of the federal poverty level . In 2020 that number will be $49,460 for an individual, $67,640 for a couple and $103,000 for a family of four. The state of California will supplement those subsidies for taxpayers with higher incomes, up to 600 percent of federal poverty level.
Recommended Reading: Ways To Make Money Unemployed
Q If I Have Private Health Insurance Can I Be Eligible For Medicaid
A. It depends. If your income is low, and you have minor children, you and your children can have private health insurance and still be eligible for Medicaid. Certain Medicaid qualifying programs require that you not have any other health insurance in order for you to get Medicaid. If you have both private health insurance and Medicaid, you should show both your Medicaid card and your private health insurance card to your medical provider each time you receive services.
What Counts As Income When Youre Enrolling In Health Insurance
Figuring out what sources of income to include in applications for Medicaid and Marketplace coverage can be confusing and overwhelming. For the most part, most taxable and nontaxable sources of income are counted when deciding Medicaid eligibility and financial savings for the Marketplace. However, there are a few exceptions. Read more below.
Also Check: How Do I Track My Unemployment Card
Medicaid Chip And Insurance Plans Through The Marketplace
When you fill out a Marketplace application, youll find out if you qualify for any of these types of coverage:
- A Marketplace insurance plan. You may qualify for premium tax credits and savings on deductibles, copayments, and other out-of-pocket costs based on your household size and income. Some people with low incomes may wind up paying very small premiums. Learn about getting lower costs on a Marketplace insurance plan.
- Medicaid. Medicaid provides coverage to millions of Americans with limited incomes or disabilities. Many states have expanded Medicaid to cover all people below certain income levels. Learn more about Medicaid and how to apply.
- Childrens Health Insurance Program . CHIP provides coverage for children, and in some states pregnant women, in families with incomes too high for Medicaid but too low to afford private insurance. Learn more about CHIP.
After you finish your Marketplace application, youll get an eligibility determination that tells you what kind of coverage you and others in your household qualify for.
Q Who Qualifies For Medicaid
A. Citizenship and Residency – To obtain full Medicaid benefits in Delaware, you must be a Delaware resident and either a U.S. citizen or a legally residing noncitizen. Full coverage for noncitizens which include DACA recipients is dependent on the availability of state funding. However, noncitizens can qualify for coverage for emergencies and labor & delivery services if income requirements are met.
Income Level – Qualifying for Medicaid is also based on need. Household income must be under certain limits as defined by the Federal Poverty Level and is based on family size. For Long Term Care programs, financial resources must also be under a certain amount. There are also specific programs for individuals who meet certain medical or disability tests, or who qualify due to age or pregnancy. To find out more about different Medicaid and other medical assistance programs, visit DMMA Programs & Services.
Read Also: Are Unemployment Benefits Delayed On Holidays 2020
What If Im Turned Down By Medicaid
- You may be able to buy a private health plan through the Marketplace instead for the 2018 plan year in the fall. You may qualify for savings based on your income through a premium tax credit and savings on out-of-pocket costs.
- If you don’t qualify for either Marketplace or Medicaid savings, you still have options. Learn more here.
What Happens To Your Employer
If you are laid off from your job, your health insurancecoverage typically ends when your job does. Some employers will extend benefitsto the end of the month in which you are laid off, but this varies from companyto company. Under a federal program known as COBRA, you may keep your currentinsurance, but you must pay the full amount of the premiums and any otherexpenses previously covered by your former employer.
The cost of keeping your current coverage under COBRA can bequite high. Many individuals find it is more cost-effective to enroll in anunemployed health insurance plan that will offer similar coverage for lessmoney in many cases.
Don’t Miss: Are Unemployment Benefits Delayed On Holidays 2020
Medicaid Coverage With Other Benefits During The Covid
12. I turned 65 but haven´t been able to apply for benefits such as Medicare or Social Security due to the COVID-19 emergency. Will my current Medicaid coverage be affected?
- No. During the COVID-19 emergency you will not be required to apply for other benefits, such as Medicare or Social Security.
13. I have been unable to complete my application for Veterans Benefits due to the COVID-19 emergency. Will I be able to enroll in or keep my Medicaid coverage?
- Yes. During the COVID-19 emergency, you will not be required to apply for Veterans Benefits.
14. I have been unable to provide my local district with Third Party Health Insurance information, including that my TPHI has ended. What should I do?
- You will not be required to provide TPHI information in writing, but tell your local district if your insurance has ended or if there are any other changes to your TPHI.
15. I was making voluntary re-payments for overpayments I received as reimbursement for my Third Party Health Insurance but I am unable to make the payments right now due to the COVID-19 emergency. What should I do?
- You may stop making re-payments, and start them again as soon as you are able.
16. I am in the Medicaid Buy-In Program for Working People with Disabilities program, and I lost my job due to the COVID-19 emergency. Will I lose my Medicaid coverage?
Medicaid Expansion For The Unemployed
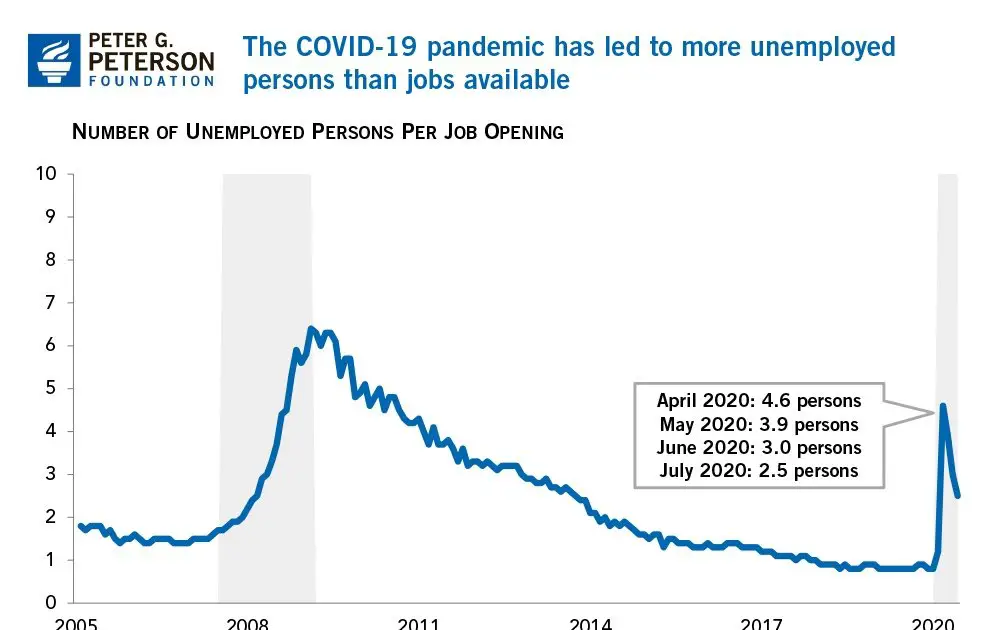
Under the Affordable Care Act, states have the option to expand Medicaid to families with incomes up to 138 percent of the federal poverty level. To rapidly absorb the unemployed into affordable coverage, states should have the option to further expand Medicaid to two categories of enrollees: 1) individuals who are receiving unemployment insurance benefits or who were receiving unemployment insurance benefits that expired during the public health emergency and 2) families with incomes up to 200 percent of the federal poverty level. As under the current Medicaid program, eligible individuals who are enrolled in ACA coverage or employer coverage would be able to switch to Medicaid.
For the first eligibility category, states would automatically enroll in Medicaid all individuals who receive unemployment insurance benefits or food stampsunder the Supplemental Nutrition Assistance Program regardless of their income. This auto-enrollment would be similar to the current Express Lane Eligibility option, in which several states enroll children in Medicaid or the Childrens Health Insurance Program based on their SNAP eligibility.
States would guarantee continuous eligibility for these enrollees until the end of the public health emergency, at which point their eligibility would be redetermined. If they are no longer receiving unemployment insurance benefits, they would qualify for Medicaid under the second eligibility category.
Read Also: What Day Does Unemployment Get Deposited In Nc
Q How Do I Join A Managed Care Organization
A. After being notified that you are eligible for Medicaid , you will receive in the mail a packet of information about the different MCO plan options for receiving your Medicaid benefits. You may choose any plan described in this mailing. You probably want to choose a Managed Care Organization to which your doctor belongs. If you need help making this decision, call the Health Benefit Manager at the phone number in the mailing.
Affordable Care Act Subsidized Plans After Medicaid
Special Enrollment Status: If you lose your Medicaid health coverage, a Special Enrollment Period opens up for you. During an , you can obtain full-featured health insurance known as an Affordable Care Act plan.
The SEP is only a 60-day window, so you have to act quickly. Tools like HealthCare.com help you determine which plan is best for your needs and budget.
Without a Special Enrollment Period, you can enroll in a health plan only during the annual Open Enrollment Period, which generally lasts from November 1 through December 15. Once the window closes, you will be unable to enroll in healthcare coverage until the next open enrollment period.
For example, if your Medicaid is canceled as of March 1, you will have 60 days to enroll in a health plan through Obamacare. If you dont enroll by the end of that 60-day window, you will have to wait until the next open enrollment period, and the coverage would not be effective until January 1 of the following year.
If you know when your Medicaid plan ends, you can sign up in advance. Health insurance plans are generally effective the first day of the following month after you apply, but a new application may take some time to process.
ACA Discounts for Low and Moderate Incomes: The cost of health insurance premiums can be intimidating, but help is available. Depending on your income level, you might receive a subsidy for ACA coverage.
Recommended Reading: Unemployment Holiday Delay 2020
Who Is Eligible For Medicaid
Medicaid has somewhat different eligibility criteria in every territory and state, but all state-level programs use federal guidelines as a starting point for approval of applicants. As a rule, Medicaid enrollees must be:
- U.S. citizens or permanent legal residents who meet length-of-residency requirements
- Residents of the state where the application is submitted
- Earning less than the state maximum income and have less than the maximum countable assets, which does not include a single home or car
- Free from past convictions for benefits fraud, not have voluntarily surrendered access to benefits in lieu of prosecution or have any other disqualifying civil or criminal history
Income verification is usually part of the Medicaid application process. To establish an applicants income, program workers often look back over a period of 60 months to see how much money you earned. In California, the look back period is 30 months. This assessment helps to determine whether you earn too much money to qualify for Medicaid benefits. It also helps to establish how much of a share-of-cost you should have before your Medicaid benefits kick in, if any.
Gaps In Health Coverage
The pandemic and economic crisis have exposed major gaps in health coverage. Individuals who lose their jobs and employer coverage could fall through four cracks:
You May Like: Are Unemployment Benefits Delayed On Holidays
Do I Qualify For Medicaid
Medicaid provides free or low-cost health coverage to some low-income people, families and children, pregnant women, the elderly, and people with disabilities. Many states have expanded their Medicaid programs to cover all people below certain income levels. Medicaid qualifications depend partly on whether your state has expanded its program.
What About The Money I Was Supposed To Receive From Earlier Months
Details are being worked out. We anticipate it working like this: If you were enrolled through the State Exchange on a discounted Covered California plan as of January 1, 2021, then you will qualify for the unemployment discount for the whole year. The discounts you did not receive for prior months will result in you getting extra money back on your taxes when you file in 2022 for tax-year 2021.
Perhaps you did not enroll through the exchange for January 1, but you still have prior months in 2021 on subsidized coverage. In that cast, those prior months should cause you to qualify for extra discounts that will be reconciled when you file your taxes next year.
If you had not previously been on discounted health insurance through Covered California, then we expect that you will not receive the discounts for previous months. However, we expect that you should be able to get the discount from August through to the end of the year.
Recommended Reading: Can Llc Owner Collect Unemployment
Cost And Coverage Of Medicaid In New York
Estimates for the cost of Medicaid can vary depending on things like the individual patient and services needed. These copays will be small. People who will receive free healthcare from Medicaid include those who are under the age of 21, women who are pregnant, and patients who are in long-term care.
As far as coverage goes, Medicaid typically pays for most medical services, along with any medications and supplies that are needed. This includes coverage for things like:
- Family planning services and prenatal care
- Ambulance rides to the hospital in emergency situations
- Public transportation or car mileage to the patients medical appointments
- Medicines, supplies, medical equipment, and appliances
- Early screening, diagnosis, and treatment for beneficiaries who are under 21
- Other various services that might be needed
Can You Have Both Medicare And Medicaid

Yes, you can qualify for coverage under both programs at the same time. When this occurs, it is called dual eligible. This generally applies when a person is over 65 or disabled and has very limited income. You still have the choice to enroll in Original Medicare or a Medicare Advantage Plan. When a person is dual eligible, most of their medical expenses are completely covered by one or both of the programs. Medications are generally covered through a Medicare Part D prescription drug plan, although Medicaid may cover additional medications or other medical services that are not covered through Medicare.
If you are eligible for both government programs, then it is usually a good idea to enroll in each. Go ahead and sign up for Medicare and Medicaid benefits. When enrolled in both programs, a person typically has very little out of pocket expense.
Donât Miss: Pa Unemployment Ticket Number Status
Recommended Reading: Can You File Bankruptcy On Unemployment Overpayment
Consolidated Omnibus Budget Reconciliation Act
Yeah, thats a mouthful. No wonder we just call it COBRA. To put it simply, COBRA gives you the chance to extend your employer-based coverage for a limited period of time after youve stopped working for them. Big sigh of relief, right? Here are some of the upsides and downsides:
Advantages of COBRA
The good thing about COBRA is that it makes it mandatory under federal law for an employer to allow employees to pay to stay on their health care 18 months after theyve left their job. This can also stretch to 36 months if you qualify.
Disadvantages of COBRA
The not-so-great thing about COBRA is that it does mean youll pay the full cost of the health insurance premium yourself. Youll pay more than what you saw coming out of your paycheck when you were employed because your employer was subsidizing a percentage of that health care premium.
Now, if this is going to break the bank, dont worry! You can buy individual ACA health insurance instead . But its always a good idea to speak to your employer before or as soon as you leave your job to get the lowdown on what your new COBRA premium might be. That way you have all your bases covered.
What Happens if You Change Your Mind About COBRA?
Everyones allowed to change their mind. Right? A couple of months of COBRA coverage might leave you thinking that its just too expensive. Or maybe you got another job sooner than you thought you would and dont need it anymore. What now?
